How Effective Is Oral Appliance Therapy at Treating Sleep Apnea?
Finding out that you have obstructive sleep apnea is equal parts relief and uncertainty. On the one hand, you’ve finally discovered the cause of your snoring, daytime sleepiness, and cognitive changes. On the other hand, you’re left with a choice, should you use CPAP or oral appliance therapy to treat your sleep apnea?
Through this uncertainty, remember that in treating your obstructive sleep apnea, you’re lowering your risk for sometimes fatal health consequences such as heart disease, stroke, and dementia. Whichever sleep apnea treatment you choose, make sure that you’ll wear it so you can live a happy, healthy life.
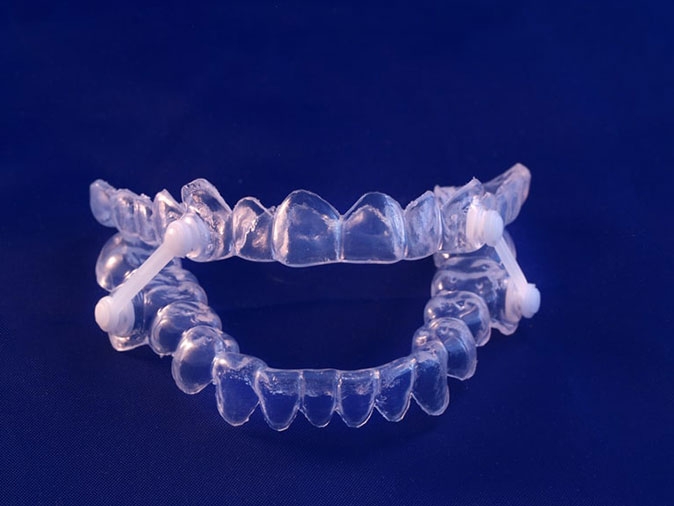
Effectiveness: CPAP vs. Oral Appliance Therapy
How effective is oral appliance therapy at treating sleep apnea? While this may seem like a simple question, it can get complicated. In clinical studies with groups of people with 100% adherence to CPAP and oral appliance therapy, CPAP comes out victorious.
CPAP is 100% effective in treating obstructive sleep apnea, from mild to severe. In observational studies, oral appliance therapy effectiveness has been shown to be anywhere from 52% to 97%.
However, this is where things can get complicated. The real-world effectiveness of oral appliance therapy is equal to or higher than CPAP due to people not sticking to treatment with CPAP. This is for various reasons, such as people finding CPAP uncomfortable to wear, too loud, or experiencing side effects like daytime bloating. Due to this, oral appliance therapy is just as effective as CPAP.
An article published in the National Library of Medicine examined studies looking at the long-term effectiveness of oral appliance therapy vs. CPAP. Here are the important points to consider when determining what’s best for you.
- Over 5 years, treatment outcomes for both oral appliance therapy and CPAP were equally as effective at reducing the likelihood of fatal cardiovascular events in those with severe obstructive sleep apnea.
- Oral appliance therapy proved just as effective as CPAP in reducing blood pressure, endothelial function, and microvascular reactivity. Researchers surmise that this and the above point are due to patients’ higher adherence to oral appliance therapy.
- Both treatments improved quality of life in a disease-specific questionnaire; however, in a general questionnaire about quality of life using the treatment, oral appliance therapy won.
- The study examined in this article found that people with a high BMI withdrew from using oral appliance therapy and switched to CPAP.
- Researchers believe that oral appliance therapy is an effective alternative treatment to CPAP unless a person’s BMI is too high.
Which is best for you?
When it comes to which obstructive sleep apnea treatment is best for you, researchers have an answer for that too. Historically, doctors would first prescribe CPAP, and then only if patients couldn’t adhere to treatment would they prescribe oral appliance therapy. According to research, that may not be the best route.
In both CPAP and oral appliance users, adherence to treatment was higher when patients could choose which treatment they wanted rather than being prescribed one option. This choice lets patients feel in control of their treatment, making them more likely to stick to the treatment, resulting in fewer sleep apnea symptoms and a lower risk of developing other conditions.
Leaving the choice up to you may still leave you wondering which option is truly the best. But here are some things to consider.
- The severity of obstructive sleep apnea (OSA): Those with mild to moderate OSA can feel confident in choosing oral appliance therapy. Those with severe OSA may want to start with CPAP.
- Comfort: CPAP isn’t comfortable for everyone. If you think that’ll be an issue, consider oral appliance therapy. However, be aware that oral appliance therapy takes some getting used to also.
- Budget: Oral appliance therapy is more cost-effective than CPAP.
- Travel: You can travel with a CPAP machine, but you’ll need to ensure you’ll have electricity. If you won’t have electricity, consider oral appliance therapy. Even if it’s a “once in a while” treatment when camping.
- Jaw and TMJ: Oral appliance therapy moves your jaw forward, which could result in pain in your jaw joint. However, this can be avoided by choosing a neuromuscular dentist to create your appliance.
How to Get Obstructive Sleep Apnea Treatment
The first step in getting treatment is to seek a diagnosis. SleepTest.com can help you with that.
We offer sleep studies that you can conduct in the comfort of your own home, on your own time. The two-night study should be conducted consecutively, and then you’ll send your results back to SleepTest to be analyzed by a sleep doctor. You’ll consult with your sleep doctor via the patient portal and online appointments.
After you receive your diagnosis, talk with your doctor about what may be best for you. If you choose to go the oral appliance therapy route, you’ll be referred to a neuromuscular dentist who can fit you with an oral appliance. The only step after that is to use your oral appliance each time you sleep.

Feeling tired all the time, even after a full night’s sleep? You might be suffering from sleep apnea. Discover how an at-home sleep test can help diagnose the root cause of your fatigue—and get you back to feeling like yourself.

Spring is here—and so is the pollen. For the millions dealing with seasonal allergies, the symptoms can be more than just annoying. And if you also have sleep apnea, those stuffy nights and restless sleep can get even worse.
Let’s take a closer look at how spring allergies and sleep apnea affect each other—and what steps you can take to sleep more comfortably.




